Unit 8: Metabolic and Endocrine Health Alterations
8.1 Overview | 8.2 Unit Learning Outcomes | 8.3 Metabolic Disorders | 8.4 Endocrine System Disorders | 8.5 Fluid and Electrolytes | 8.6 Assignment 2 | 8.7 Closing Reflections | 8.8 References

8.1 Overview
The focus of this unit is on care of patients with alterations in metabolism related to pancreatic, biliary, hepatic, and endocrine disorders. One in four Canadians— across the lifespan— may be affected by liver disease, and the most common liver disease in Canada, affecting over 7 million people, is non-alcoholic fatty liver disease (Canadian Liver Foundation, 2017). Liver cancer is on the rise and is one of the most serious cancers in Canada (Canadian Liver Foundation, 2017).
According to Lewis et al., (2014) the primary cause of acute pancreatitis in Canadians is gallstones and the second most common cause is alcohol abuse. Gallstones, or cholelithiasis, can be a cause of acute pancreatitis and obstructive jaundice (Lewis et al., 2014). The development of cholelithiasis and cholecystitis has some relationship to sedentary lifestyle and obesity (Lewis et al., 2014).
All of these alterations in metabolism have some connection to modifiable risk factors. Pancreatitis, hepatitis, and cirrhosis of the liver are all potentially life threatening. Patients with these types of health alterations need pain and nausea management, nutrition and hydration to support body functions, and assistance with lifestyle modifications (Paul et al., 2016). Patient education and counseling are critical nursing interventions.
8.2 Unit Learning Outcomes
After completing Unit 8, you will be able to:
- outline safe and effective nursing care of patients with alterations in nutrition and hydration related to illness and/or injury including metabolic related pancreas, biliary, hepatic, and endocrine disorders;
- summarize effective nursing management of patients with endocrine disorders including diabetes mellitus, and disorders related to the thyroid, pituitary, parathyroid, and adrenal glands;
- interpret laboratory and diagnostic results, effects of pharmacological therapy in the management of patients with metabolic and endocrine disorders;
- describe the fundamentals of fluid and electrolyte balance and how these influence health; and
- summarize the steps for administration of intravenous (IV) fluids and medications.
8.3 Nursing Care of Patients with Metabolic Related Pancreas, Biliary and Hepatic Disorders
Ensure at a minimum you know:
- the physical assessment of liver function;
- the diagnostic and laboratory evaluations including liver function tests, CT, MRI;
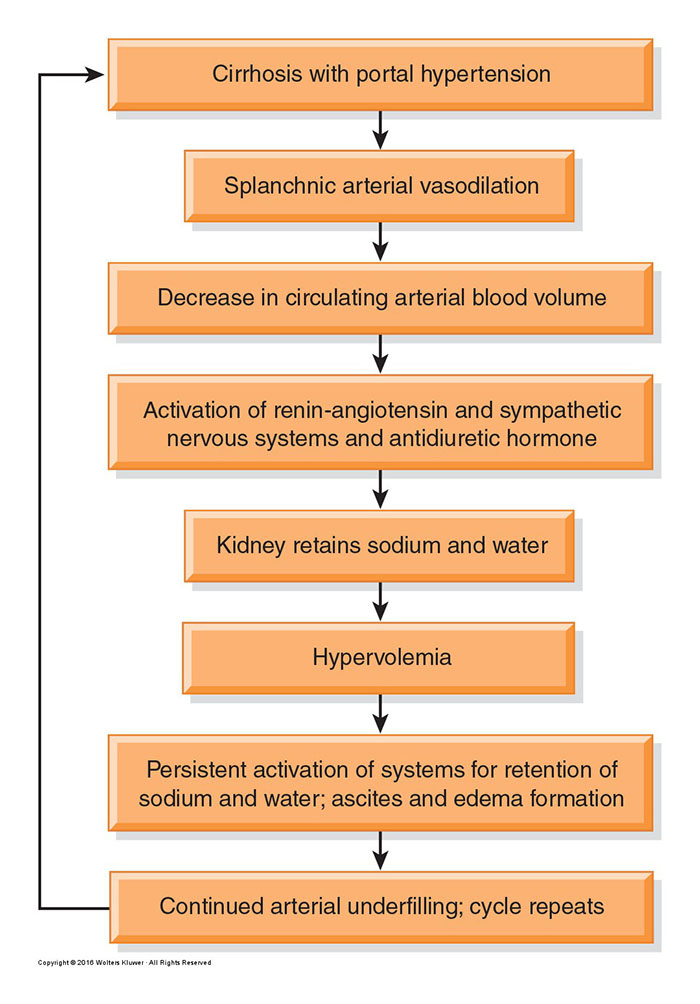
- the clinical manifestations and nursing management of hepatic dysfunction including: jaundice, portal hypertension, ascites, esophageal varices, and hepatic encephalopathy;
- the clinical manifestations and management of types of hepatitis, cirrhosis, and cancer of the liver; and
- the clinical manifestations and management of disorders of the gallbladder and pancreas including pre/post diagnostic procedures and surgery.
Learning Activities
1. Review the chapters in the course textbook on the assessment and management of patients with hepatic and biliary disorders.
2. Review the various Student Resources related to the textbook in thePoint® .
Supplemental Learning Activities
1. Mastery Level Quizzes Complete mastery practice quizzes in the following Nursing Topic Chapter in PassPoint : Metabolic Disorders.
2. Some resources that you might find useful:
Liver Cirrhosis Nursing Care Plan & Management
5 Pancreatitis Nursing Care Plans
Clinical Practice Guidelines for Liver Disease
8.4 Nursing Care of Patients with Endocrine System Disorders

Ensure at a minimum you know:
- the physiology, pathophysiology, clinical manifestations, management, complications, and pharmacologic and nutritional treatments of different types of diabetes;
- about insulin therapy, preparation, and administration;
- the common antihyperglycemic agents
- how to provide diabetic teaching;
- the acute complications including hypoglycemia, diabetic ketoacidosis, HHNS;
- the long term complications of diabetes mellitus including nephropathy, neuropathy, foot and leg problems;
- the significance of Basal Bolus Insulin Therapy (BBIT);
- the assessment of a patient with an endocrine disorder;
- the clinical manifestations, diagnostics, and therapies of patients with disorders of the pituitary and thyroid glands (diabetes insipidus, SIADH, hypothyroidism, hyperthyroidism, thyroid storm, thyroiditis, tumours, goitre);
- the role of hormones such as thyroid hormone, calcitonin;
- the clinical manifestations, diagnostics, and therapies of patients with disorders of the parathyroid glands (hypo/hyperparathyroidism), adrenal glands (Addison's Disease, Cushing's Syndrome); and
- the role of corticosteroid therapy.
Learning Activities
1. Review the chapters in the course textbook on the assessment and management of patients with endocrine disorders and diabetes mellitus.
2. Review the various Student Resources related to the textbook in thePoint®
3. Focus on Nursing Interventions
Review your knowledge related to the administration of insulin and management of hyper/hypoglycemia. Find resources in your clinical agency or consult a clinical skills text.
Basal Bolus Insulin Therapy (BBIT) is a method of scheduling and dosing daily insulin subcutaneous injections that better replicate the natural physiological process. Review the educational resources at Basal Bolus Insulin Therapy, where you will also find a self-study guide for nurses.4. Fill in the following compare and contrast document to understand agents to control blood glucose levels. (Word .doc file)
Compare and Contrast Prototypes drugs for Agents to Control Blood Glucose Levels
| Class & Prototypes | Therapeutic Action |
Pharmacokinetics |
Caution |
Adverse Effects |
Drug-to-Drug |
Insulin |
|
|
|
|
|
Sulfonylureas |
|
|
|
|
|
Other Antidiabetic Agents
|
|
|
|
|
|
Glucose-Elevating Agents |
|
|
|
|
|
5. Medication Math Moments: Work through the following two case scenarios.
You are also the primary nurse for Mr. Elektrolite's roommate Mrs. Exreigh, who is NPO pre-operatively for a bowel resection. Mrs. Exreigh has had Type 2 diabetes for many years and she has been having trouble monitoring her blood glucose and medications. You are concerned about her blood glucose reading of 16.7. The medical team decides to start Mrs. Exreigh on a continuous IV infusion of insulin to control her hyperglycemia and support her NPO status pre-operatively.
Complete the following. Include the units of measurement in your answers. Click on the question to see the answer.
As per the patient care orders, you prepare a solution of 100 mL of normal saline with 100 units of regular insulin. What is the concentration of this solution (unit/mL)?
1 unit/mL
100 units/ 100 mL = 1 unit/mL
You initiate the infusion at 1.5 units/hr as per the patient care orders. What flow rate (mL/hr) will you program into the IV pump?
1.5 mL/hr
1.5 units = 1 unit => 1.5 units.mL = 1 units.hr => 1.5 mL/hr
hr mL
You also initiate via Y-connection a solution of D10W at 80 mL/hr and a separate IV hydration solution of normal saline (0.9 % sodium chloride). If the patient care orders specify that a total IV fluid per hour is 100 mL/hr, then what is the flow rate (mL/hr) for the normal saline infusion?
18.5 mL/hr
100 mL/hr - (80 mL/hr + 1.5 mL/hr) = 18.5 mL/hr
You repeat Mrs. Exreigh's capillary glucose in 1 hour and it is now 15.0. As per the patient care orders, you need to increase the infusion by 0.5 units/hr. What is the new flow rate (mL/hr) you will program into the IV pump?
2 mL/hr
1.5 mL/hr + 0.5 mL/hr = 2 mL/hr
Which other infusion will you need to adjust based on this information?
Adjust normal saline to 18 mL/hr
100 mL/hr - (80mL/hr + 2 mL/hr) = 18 mL/hr
Mrs. Exreigh informs you she is nauseous. As per her prn orders, she is able to have dimenhydrinate 50 mg IV/IM every 6 hours for nausea as needed. You decide to administer the medication intramuscularly. Dimenhydrinate is available in 50 mg/mL ampoules. How much will you draw up into your syringe for the dose?
1 mL
50 mg = 50 mg => x mL = 1 mLContinuing with the above question, what size of needle will you use for the IM injection?
The needle length should be based on the site for injection and patient's size and age. "The viscosity of the medication, injection site, patient's weight, and amount of adipose tissue influence needle size selection. Determine needle gauge by the medication to be administered" (Perry, Potter, & Ostendorf, 2018, p.600). 5/8'' to 1 ½ " and 20- 25 gauge
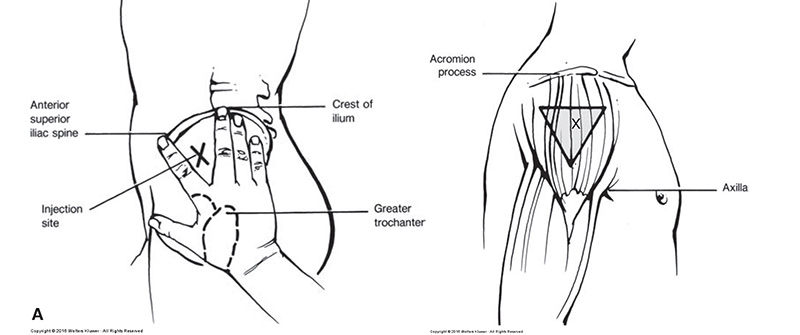
Where might you administer this medication?
Ventrogluteal and deltoid are preferred sites for adults. The ventrogluteal site is the safest and most preferred site for adults and especially for volumes greater than 2 mL (Perry, Potter, & Ostendorf, 2018). The deltoid site is easily accessible and may be used for volumes less than 2 mL (Perry et al. 2018). As there is more potential for injury, only use this site when the ventrogluteal is not accessible (Perry et al. 2018). Always check clinical agency policies regarding administration of medications via intramuscular injection
Mrs. Exreigh's blood pressure has significantly decreased. The surgical resident decided to order a normal saline (0.9 %) IV bolus of 1L over 4 hours. What flow rate (mL/hr) would you program into the IV pump?
250 mL/hr
1000mL/ 4 hrs = 250 mL/hr
If you start the bolus at 1445, what time will it be completed?
1845
1445h + 4 hrs = 1845h
How much normal saline would have infused after 2.5 hours?
625 mL
250mL/hr = x mL/2.5 hrs => x = 250 mL x 2.5 hrs / hr = 625 mL
How much normal saline is remaining in the bag at 3 hours and 15 minutes?
187.5 mL
Convert 15 minutes to hours = 15 mins/60 mins = 0.25 hr
250 mL/hr = x mL / 3.25 hr => x = 250 mL x 3.25 hrs / hr = 812.5 mL is infused in 3.25hrs
Remaining volume = 1000mL – 812.5 mL = 187.5 mL
Mrs. Thomas is admitted at 1500 hours and is ordered NPO. Mrs. Thomas has type 1 diabetes. She is initiated on an intravenous infusion of D5W at 125mL/hr and an IV insulin infusion post-operatively for hyperglycemia as follows:
IV Insulin Infusion Order
Concentration: Mix 50 units of Humulin R in 500 mL NaCl (0.9%)
Initiation: Blood glucose levels greater than or equal to 7, start Humulin R infusion at 2 units/hr
Monitor blood glucose levels q1h until stable, then q2h x 24 hours.
Sliding Scale as follows:
| Blood glucose levels | Adjustment to infusion rate |
>17.5 mmol/L |
Notify physician |
>15 mmol/L |
Increase infusion by 3 units/hr |
12.6 – 14.9 mmol/L |
Increase infusion by 2.0 units/hr |
10.1 – 12.5 mmol/L |
Increase infusion by 1 unit/hr |
5 – 10 mmol/L |
Maintain infusion |
4.0 – 4.9 mmol/L |
Decrease infusion by 0.5 units/hr |
< 3.9 mmol/L |
Contact physician |
What is the concentration (unit/mL) of the Humulin R infusion?
0.1 unit/mL
50 units in 500 mL = 0.1 unit/mL
Her initial blood glucose level at 1500 hours is 10mmol/L at what flow rate would you program into the pump?
20 mL/hr
2 units /hour is required, and there is 0.1 unit per mL. = 20 mL/hour
At 1700 hours the blood glucose level was 16mmol/L. What is the new IV insulin infusion flow rate that you would program into the pump?
50mL/hr
5 units/hour is required (0.1 unit per mL solution) = 50 mL / hour
What is the total volume (in mL) of D5W that she would receive by 2300?
1000 mL
The infusion rate ordered is 125mL / hour for 8 hours total = 125 × 8 = 1000 mL
What is the total intake of IV fluids she would have received by 2300 if from 1800 to 2300 her blood glucose levels were found to be at 9mmol/L?
1340 mL
1000 mL + (20 mL + 20 mL) + (50 mL × 6 hours) = 1340 mL
Supplemental Learning Activities
1. Mastery Level Quizzes
Complete mastery practice quizzes in the following Nursing Topic Chapter in PassPoint : Endocrine Disorders.
2. Some resources that you might find useful:
Basal Bolus Insulin Therapy (BBIT)
BBIT Self-Study Guide for Nursing (albertahealthservices.ca)
8.5 Fluid and Electrolytes: What You Need to Know
Ensure at a minimum you know:
- the processes and clinical manifestations of metabolic acidosis, metabolic alkalosis, and compensatory processes.
Learning Activities
1. Review the chapter in the course textbook on fluid and electrolyte: balances and disturbances.
2. Review the various Student Resources related to the textbook in thePoint® .
Supplemental Learning Activities
1. Additional resources you may find useful:
8.6 Assignment 2
Concept Map and Case Analysis: Nursing Care of Patients with Exocrine, Pancreas, Biliary, and Hepatic Disorders
Use the textbook chapters and other sources of evidence to create a concept map of this case scenario.
See |Assessment Overview| Once completed, submit to Assignment 2 Drop Box. You may want to go back to Unit 1 and review the content regarding concept map development.8.7 Closing Reflections
Has your view of the role of the RN changed since you started NURS 400? Review this poem called (I am a nurse) about being an exemplary nurse and reflect on your current thoughts about the difference between the LPN and RN roles. Share your insights in a journal or in the Unit 8 Forum.
I am your Nurse
I am your nurse.
I ease your pain.
I bathe your skin.
I make your bed.
I help you dress.
I meet your needs.
You heal me.
I am your nurse.
I feed you meals.
I give you rest.
I tend your wounds.
I sense your suffering.
I answer your questions.
You teach me.
I am your nurse.
I know your pain.
I share your loneliness.
I feel your despair.
I taste your joy.
I sense your spirit.
You touch my soul.
And sometimes,
for just a moment,
I am you,
and you are me,
and we are one.
Together,
we go beyond the limits
of ordinary experience,
to live the extraordinary.
(Perry, 2009)
8.8 References
Alberta Health Services (n.d.). Basal bolus insulin therapy. Diabetes Obesity and Nutrition Strategic Clinical Network. https://www.albertahealthservices.ca/scns/Page14018.aspx
Alberta Health Services. (2021) Basal Bolus Insulin Therapy (BBIT) and improved glycemic management in hospital. Diabetes Obesity Nutrition Strategic Clinical Network. https://www.albertahealthservices.ca/assets/about/scn/ahs-scn-don-bbit-self-study-guide-for-nursing.pdf
Canadian Liver Foundation. (n.d.). Clinical practice guidelines. https://www.liver.ca/professionals/health-professionals/#clinical-practice-guidelines
Canadian Liver Foundation. (n.d.). Liver disease. https://www.liver.ca/patients-caregivers/liver-diseases/
Lewis, S., Heitkemper, M.M., & Dirksen, S. R. (2014). Medical-surgical nursing in Canada (3rd ed.). Toronto, ON: Elsevier.
McClintock, M. (2013, July 2). Fluid and electrolyte basics [Video]. YouTube. https://www.youtube.com/watch?v=gVD9N1W6mbw
McClintock, M. (2013, July 2). Fluid and electrolyte disorders [Video]. YouTube. https://www.youtube.com/watch?v=AWI8hoaUkbE
Paul, P., Day, R.A., & Williams, B. (2016). Brunner and Suddarth's Canadian textbook of medical-surgical nursing (3rd ed.). Philadelphia, PA: Wolters Kluwer.
RNpedia (n.d.). Liver cirrhosis nursing care plan & management. https://www.rnpedia.com/nursing-notes/medical-surgical-nursing-notes/liver-cirrhosis/
Vera, M. (2022, March 18). Pancreatitis nursing care plans. Nurseslabs. http://nurseslabs.com/5-pancreatitis-nursing-care-plans/
Young, W.F. (2022, September). Overview of the endocrine system. Merck Manual Professional Version. https://www.merckmanuals.com/en-ca/professional/endocrine-and-metabolic-disorders/principles-of-endocrinology/overview-of-the-endocrine-system?query=endocrine%20system
